


.svg)

Project overview
Navigating health insurance in the United States is notoriously complex. For individuals and families shopping for ACA-compliant plans, the process typically involves juggling multiple carrier websites, confusing plan structures, and a registration experience that drives users away before they ever select a policy.
A US-based healthcare startup recognized this friction as a solvable problem. The founder's vision was straightforward: build a single platform where users could compare plans from multiple carriers, complete enrollment intuitively, and manage their coverage from a single unified dashboard
The challenge was that the startup came to us with an idea, not a product. There was no roadmap, no technical specification, and no design. They knew the problem they wanted to solve and the market they wanted to enter, but needed a partner who could translate that vision into a working product quickly and cost-effectively.
That is where Darly Solutions stepped in. We ran a full discovery phase, defined the product scope, built the MVP in six weeks, and have continued to expand the platform's capabilities ever since. Today, two years later, we remain the startup's dedicated technology partner.
Client’s Review
Services








Challenges
The startup arrived without a defined product. This is both the most common and the most high-risk situation for a healthcare tech company: the regulatory environment is demanding, the user expectations are high, and the cost of building the wrong thing first is steep.
Our immediate challenge was to impose structure on ambiguity. We needed to conduct discovery, align stakeholders on scope, and produce a buildable roadmap, all before writing a single line of code. At the same time, the client had a narrow window to reach the market before the next ACA open enrollment period.
On the technical side, integrating with multiple insurance carriers proved to be the most complex engineering task. Each carrier exposes its plan data and enrollment APIs differently, with varying authentication schemes, rate limits, and data formats. Normalizing this into a single unified interface required careful abstraction and robust error handling.
Data security and compliance presented an additional layer of complexity. The platform handles personally identifiable information (PII) and protected health information (PHI) categories that impose strict requirements on how data is stored, transmitted, and accessed. Every architecture decision had to account for HIPAA considerations without slowing down development velocity.
Finally, user drop-off during enrollment is an industry-wide problem. Long forms, unclear plan comparisons, and a lack of guidance cause most users to abandon the process. Designing an enrollment flow that felt effortless while still collecting all legally required information required significant UX investment.
Our discovery phase defined the following requirements:
Strategic business needs
01 Launch a functional MVP before the ACA open enrollment window
02 Support plan comparison across a minimum of 10 insurance carriers at launch
03 Achieve a user enrollment completion rate above 70%
04 Build a platform architecture that scales to 10x users without re-engineering
05 Establish a compliant data handling framework that supports future HIPAA attestation
Technical requirements
01 Design a modular carrier integration layer to support rapid onboarding of new insurers
02 Implement a unified plan comparison engine, normalizing carrier-specific data structures
03 Achieve page load times under 2 seconds across all core enrollment screens
04 Enforce role-based access control with audit logging for all sensitive data operations
05 Enable automated document generation (enrollment confirmations, plan summaries) in under 3 seconds
06 Integrate payment processing for premium collection with full PCI-DSS compliance via Stripe
07 Build an internal admin dashboard for the client's operations team
08 Deliver automated user communication workflows for enrollment reminders and status updates
We’ll run the discovery, define the scope, and deliver a live MVP in 6 weeks, so you can stop debating the idea and start onboarding real users.

.avif) Talk to an expert
Talk to an expert.webp)
Solutions
We approached this engagement as a true product partnership rather than a development contract. Starting from zero, we guided the client through discovery, defined a phased roadmap, delivered the core platform in six weeks, and have continued to ship new capabilities on a rolling basis. Below are the key product areas we built and continue to evolve.
.png)
.png)

Discovery & product roadmap
Before any design or development work began, we ran a structured discovery phase spanning two weeks. This included stakeholder interviews, competitive analysis of existing ACA enrollment platforms, and a regulatory review of data handling requirements specific to individual and family health insurance in the US market.
The output was a prioritized product roadmap with three phases: a six-week MVP targeting core enrollment and carrier comparison, a second phase focused on user account management and payment automation, and a third phase introducing AI-assisted plan recommendations and advanced analytics. This roadmap gave the client a clear path from idea to scalable product and the confidence to move quickly.
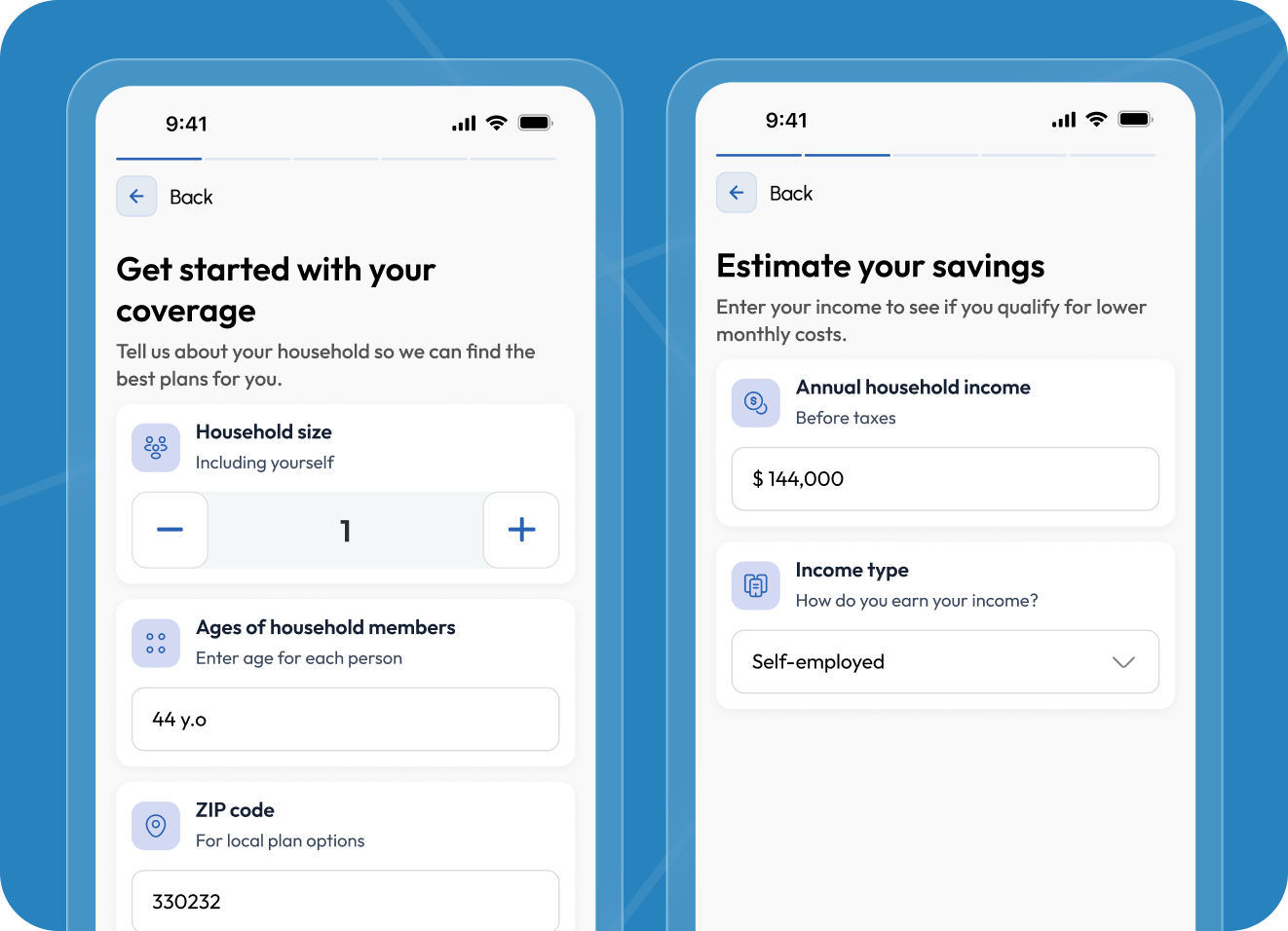
Intuitive multi-step enrollment flow
The enrollment experience is the product's most critical user-facing component. We designed a guided multi-step flow that breaks a traditionally overwhelming process into manageable stages: household information, income verification inputs, plan filtering and comparison, carrier selection, and application submission.
Each step was prototyped and tested iteratively before development, with particular attention to field validation, progress indicators, and contextual help copy. The result was an enrollment flow that users could complete in under eight minutes, well below the industry average, contributing directly to a 74% completion rate at launch.
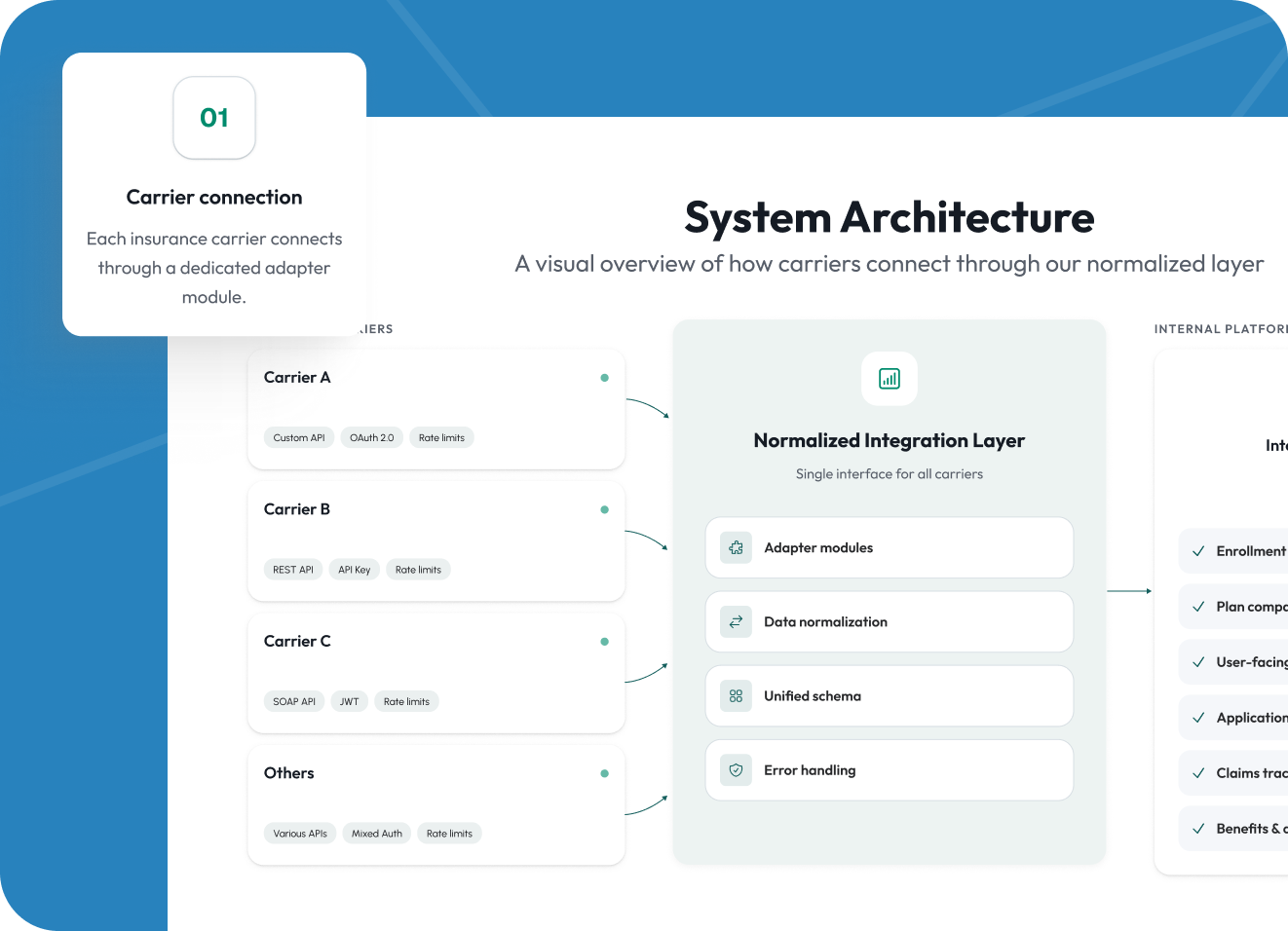
Multi-carrier integration layer
Integrating with insurance carriers is the platform's core technical challenge. Each carrier exposes plan data and accepts enrollment submissions through different APIs, with their own authentication flows, rate limits, field naming conventions, and error structures. Building a direct integration for each would have been both slow and brittle.
We architected a normalized carrier integration layer that abstracts carrier-specific implementations behind a unified internal API. Adding a new carrier requires only a new adapter module, not a re-engineering of the core application. At launch, the platform supported 12 carriers. Within twelve months, that number grew to 27, with each new integration taking an average of four days to deploy rather than weeks.

Unified plan comparison dashboard
Once a user provides their household and income information, the platform queries all connected carriers in parallel and renders a normalized comparison view. Users can filter by premium, deductible, network type, and prescription drug coverage. A side-by-side comparison mode allows direct plan evaluation across up to three options simultaneously.
The comparison engine handles the significant structural differences between carrier plan data, different field names, benefit tiers, and cost-sharing structures, and presents everything through a consistent interface. This alone represented a major differentiator versus legacy enrollment platforms that redirect users to individual carrier websites.
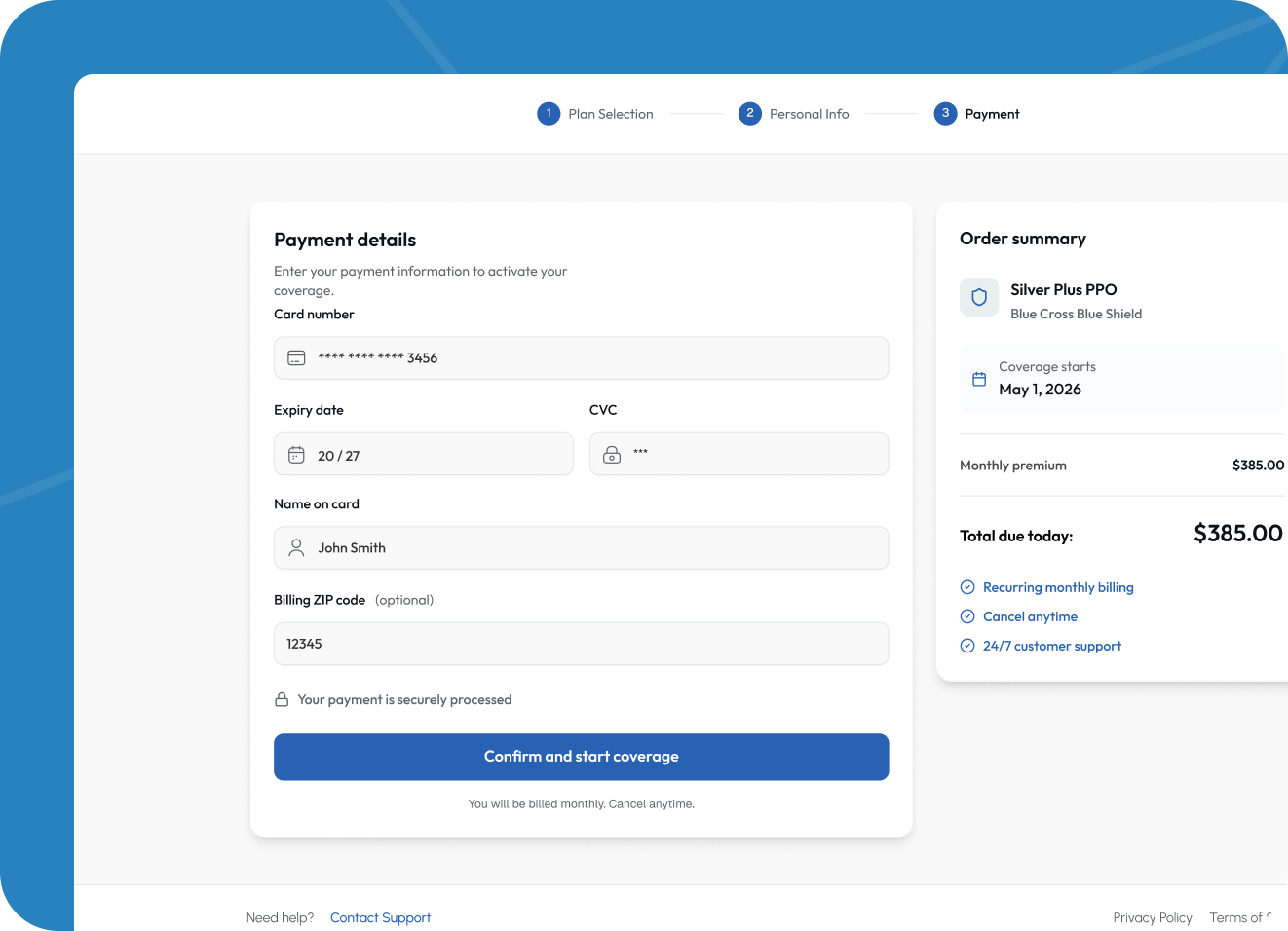
Payments and premium billing integration
We integrated Stripe to handle premium payment collection directly within the platform. Users can enter payment details once during enrollment, with the platform managing recurring monthly billing on their behalf. Stripe webhooks power automated notifications for successful payments, failed charges, and upcoming renewals.
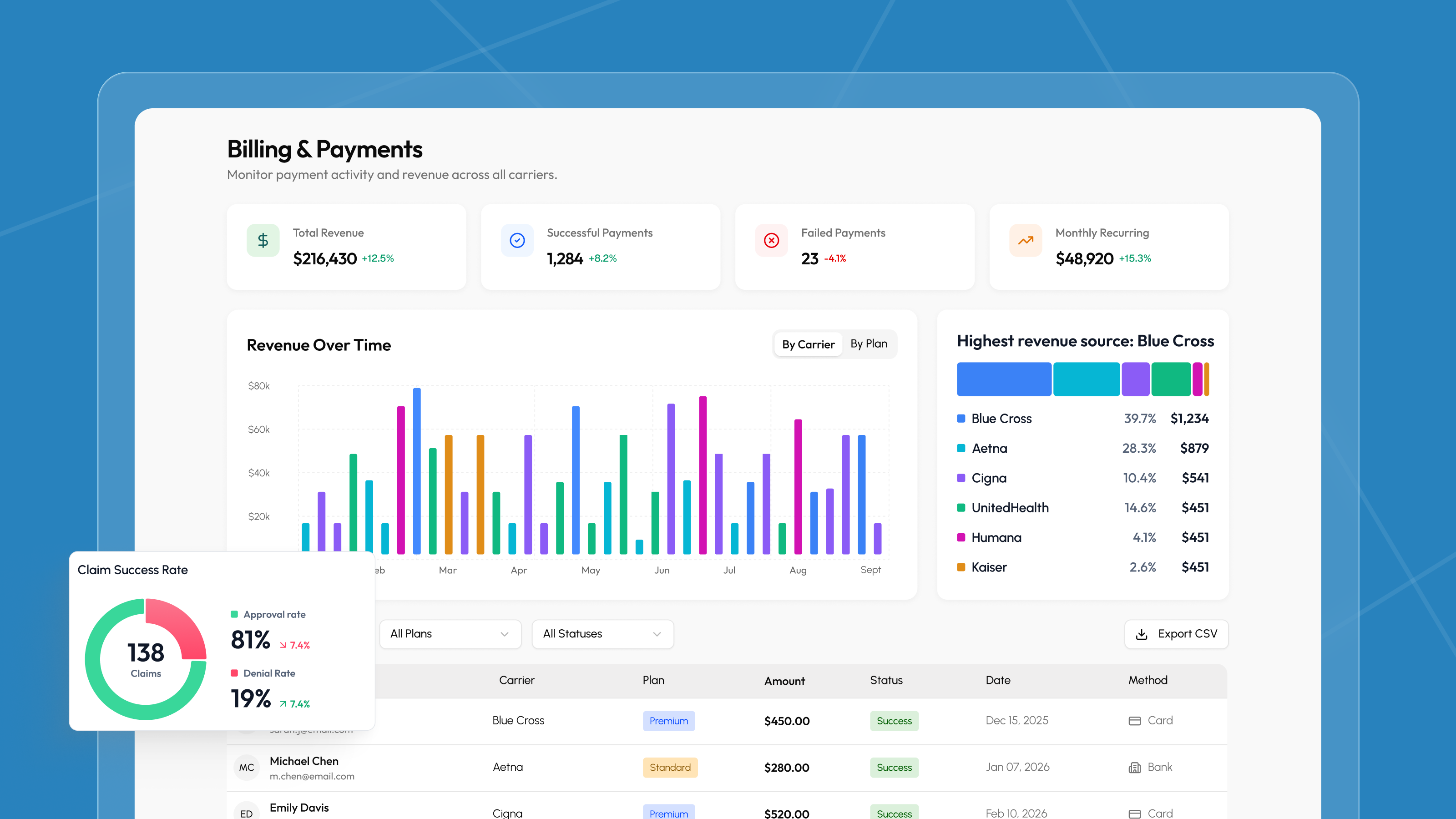
For the client's operations team, we built a billing dashboard with real-time payment status, revenue tracking by carrier and plan type, and exportable reports. This gave the startup full visibility into their revenue without requiring a separate financial tool.
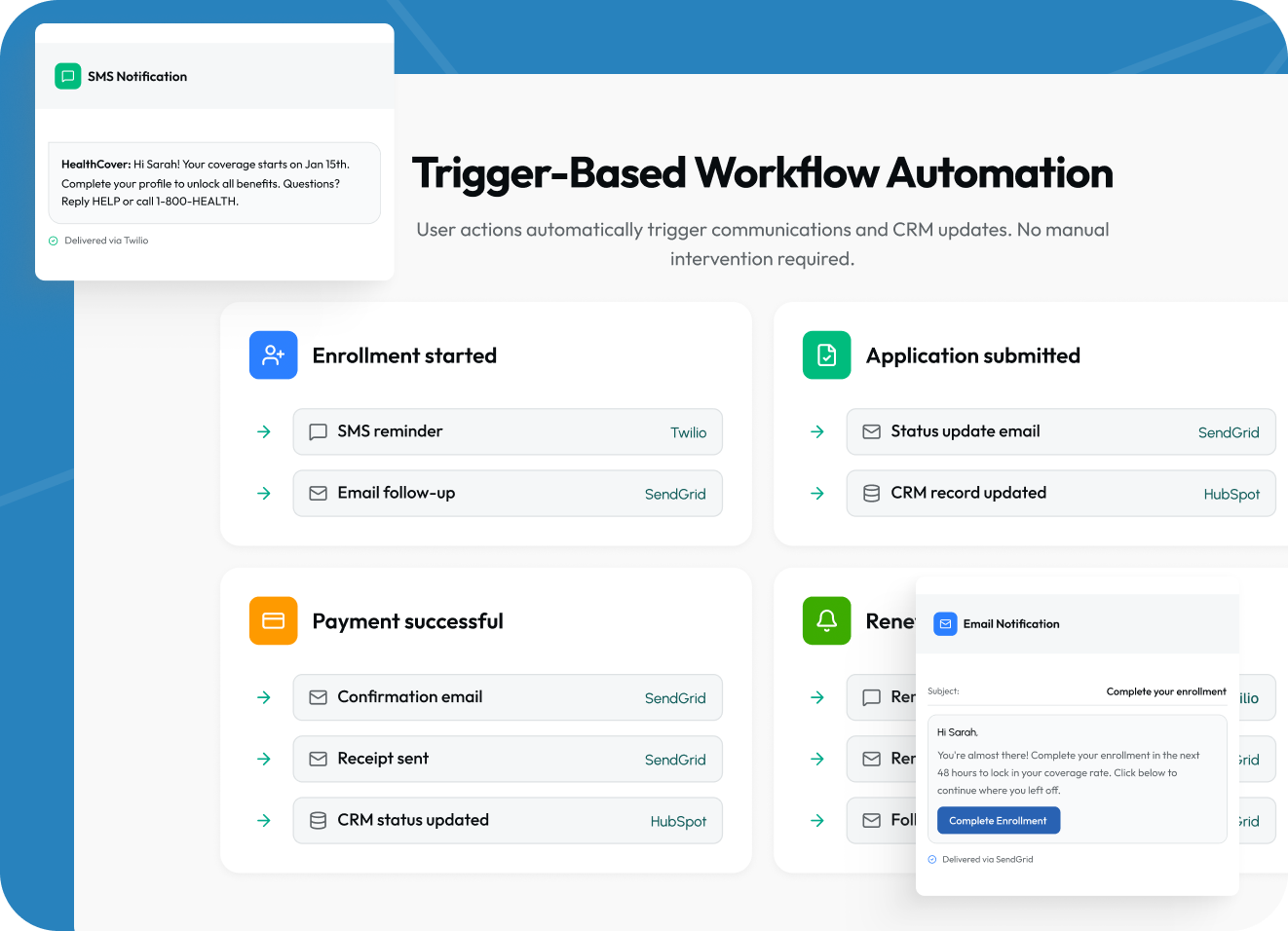
CRM, communications, and workflow automation
Insurance enrollment is not a single event — it is a lifecycle. Users need reminders before open enrollment deadlines, status updates after submitting applications, and proactive outreach when their coverage is approaching renewal. We connected HubSpot as the client's CRM backbone and built automated communication workflows using Twilio for SMS and SendGrid for email.
Trigger-based workflows handle enrollment reminders, application status changes, payment confirmations, and renewal alerts all without manual intervention from the client's team. This automation reduced the operations workload by an estimated 60% compared to managing communications manually, and contributed to measurably higher re-enrollment rates in the platform's second year.
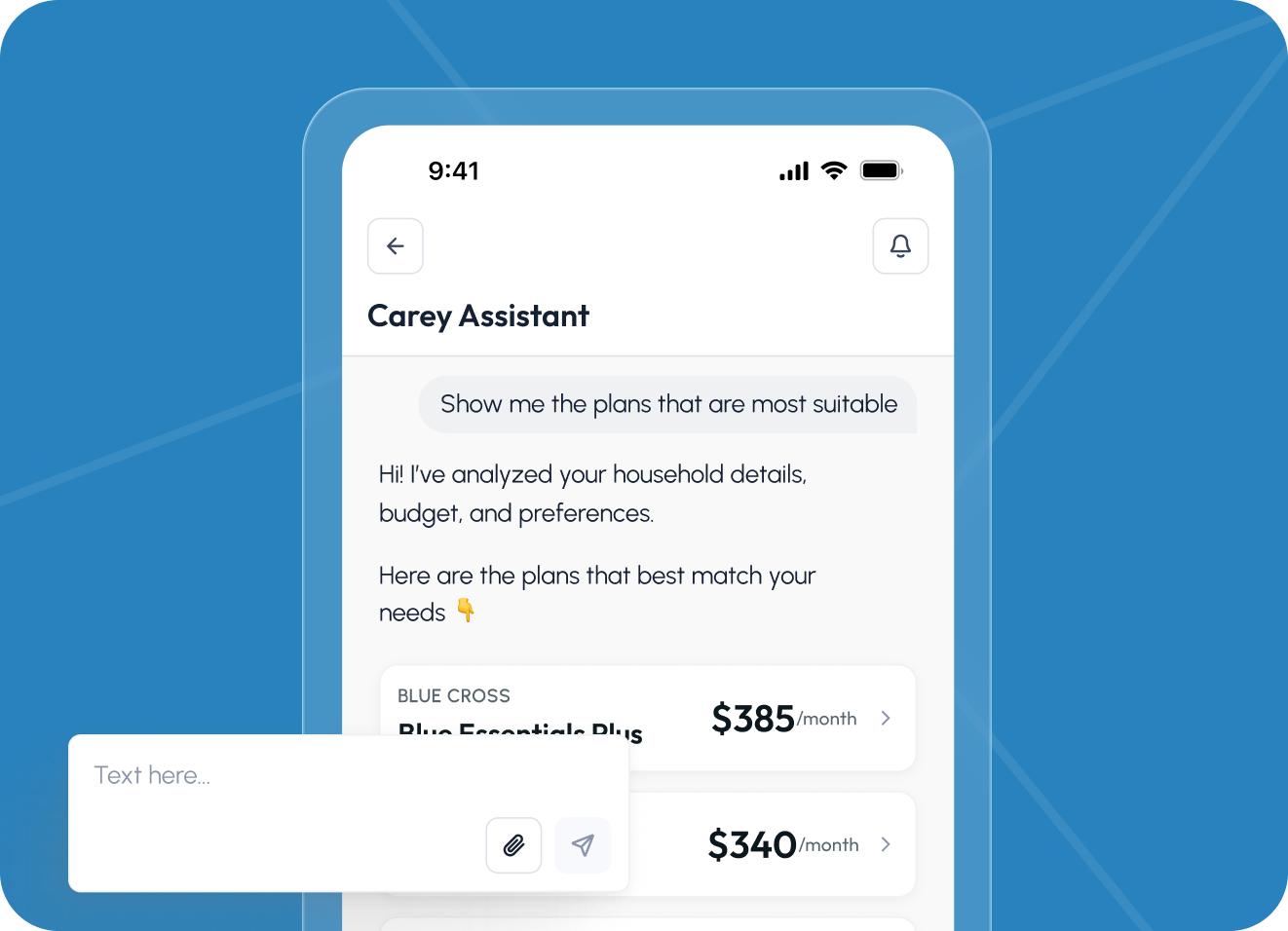
Automation and AI-assisted plan matching
As the platform matured, we introduced an AI-assisted plan recommendation feature designed specifically to operate within compliance-safe boundaries. Rather than ingesting any protected health information, the recommendation engine works exclusively with self-reported, anonymized inputs: household size, income bracket, preferred network type, and stated budget range.
Using the OpenAI API, we built a matching layer that interprets these inputs and ranks available plans by relevance, surfacing the two or three options most likely to meet the user's stated needs. The model is prompted with structured, non-identifiable data only — no PII, no PHI — making this approach safe to deploy without introducing HIPAA risk to the platform. The feature was A/B tested against the standard filter-based experience, resulting in a 31% increase in plan selection rate and a measurable reduction in time-to-enrollment.
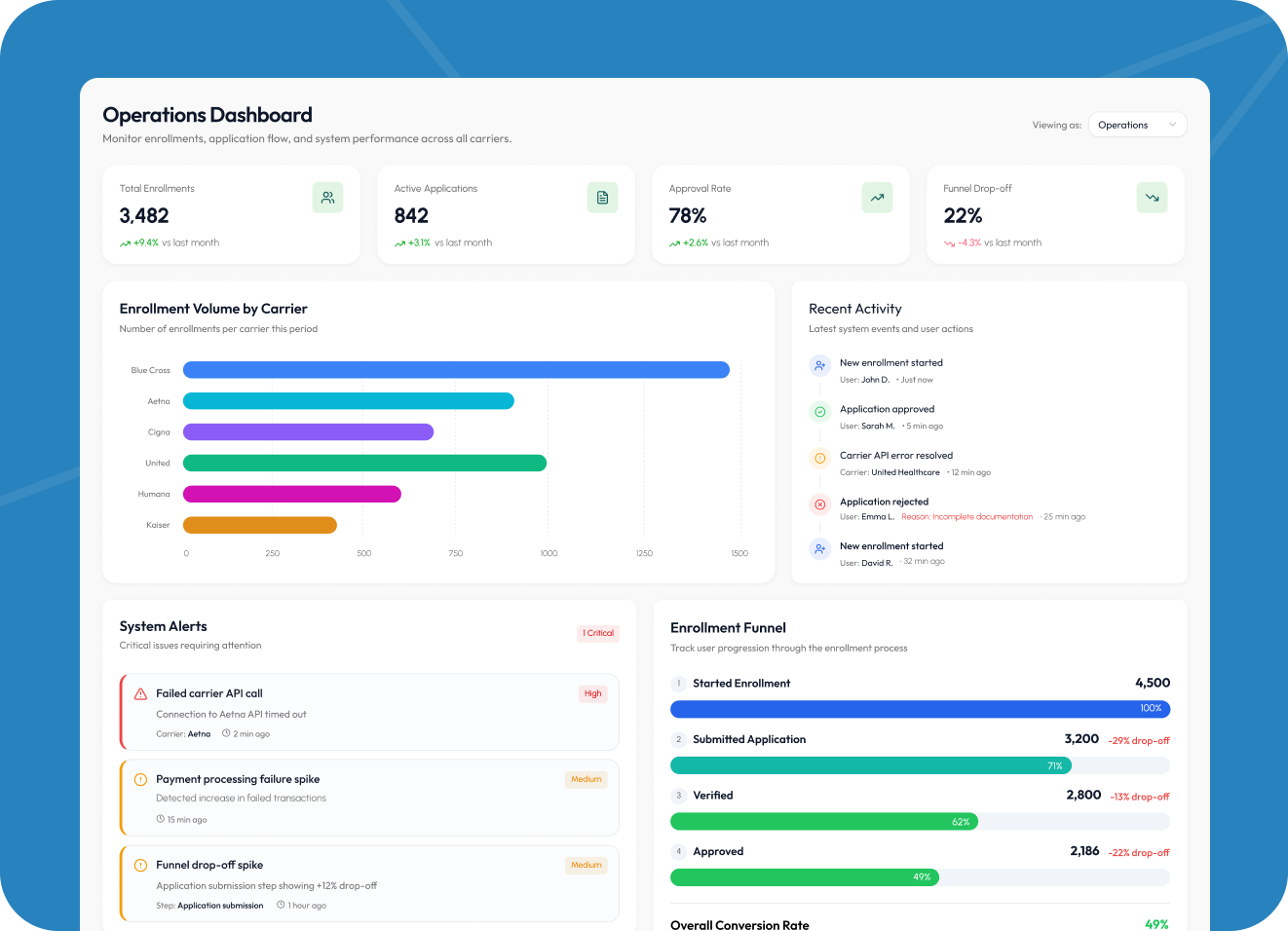
Admin dashboard and internal tooling
We built a dedicated operations dashboard for the client's internal team, providing visibility into enrollment volume by carrier, revenue by plan type, user funnel metrics, and application status tracking. The dashboard includes role-based access control so that sales, operations, and finance teams each see only the data relevant to their function.
Custom alerting notifies the team of failed carrier API calls, payment failures, and unusual drop-off spikes in the enrollment funnel, enabling the client to respond to issues before they affect users at scale.
.png)
Tech stack





.svg)
.svg)
Impact
The platform launched on schedule ahead of the ACA open enrollment window and has grown continuously since. As a result, our client received a production-ready, compliance-conscious enrollment platform that became the operational foundation for their business. Key outcomes within the first two years include:
We’ll build a modular, compliance-ready architecture that lets you onboard partners and data sources in days, maintaining high performance as your ecosystem expands.

.avif) Contact us
Contact usRelated case study
Connect with us
.webp)
We are a tech partner that delivers ingenious digital solutions, engineering and vertical services for industry leaders powered by vetted talents.












.webp)
